PRP Treatments are not currently covered by MSP, please be sure to check with your insurance provider if you are concerned with coverage.
What is PRP? (Platelet-rich Plasma)
Blood contains small solid components (red cells, white cells, and platelets.) The platelets are best known for their importance in clotting blood. However, platelets also contain hundreds of proteins called growth factors which are important in the healing of injuries.
- This in-depth article explains PRP therapy in detail.
- Here is the Wikipedia entry for Platelet-rich Plasma.
PRP is blood plasma with a concentrated number of platelets. The concentration of growth factors can be up to ten times more than is otherwise typically present.
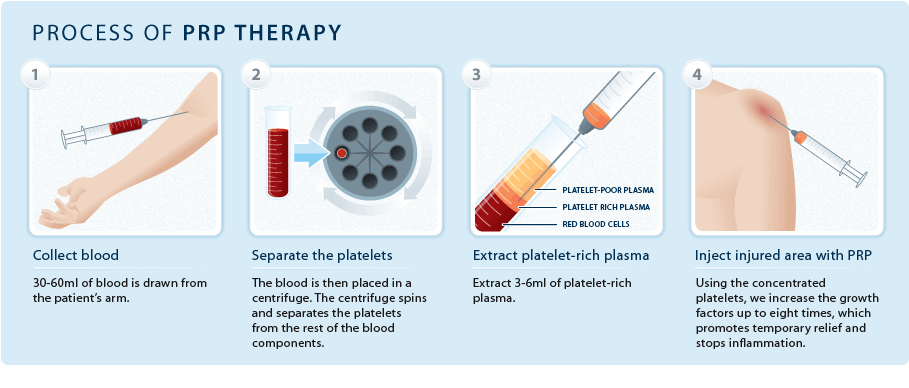
Blood must first be drawn from a patient. The platelets are separated from other blood cells and their concentration is increased using a special centrifuge. Then the increased concentration of platelets is combined with the remaining blood.
How PRP works:
PRP works by delivering growth factors to the site of an injury, and by stimulating inflammation into generating a healing response that may deliver improved timelines for healing specific types of tendon, ligament, and muscle injuries. It can be used on its own to aid the body’s own natural ability to repair itself, or as an augmentative process during surgery to improve the odds of a good outcome.
PRP injection is an extremely low-risk procedure, with potential complications similar to that of a cortisone injection in frequency of occurrence and severity.
What conditions can benefit from PRP?
- Chronic tendon injuries are among the most successful PRP treatment candidates. Tennis elbow and Jumper’s knee present types of injury well suited for this treatment.
- Ligament and Muscle Injuries are also potential opportunities to utilize PRP. Professional athletes have been using PRP to reduce healing times for common sports injuries like thigh and knee sprains; efficacy of the treatment is also influenced by the patients overall health.
- Surgical procedures utilize PRP to assist in the healing of repairs performed on torn tendons or ligaments.
- There is also potential for PRP to be useful for osteoarthritis in place of Hyaluronic Acid, or in healing certain bone injuries.
Want to learn more?
Please check out the following links for further reading:
(RESEARCH: Intra-articular Autologous Conditioned Plasma Injections Provide Safe and Efficacious Treatment for Knee Osteoarthritis)
Platelet-rich plasma (PRP) injections have become an intriguing treatment option for osteoarthritis (OA), particularly OA of the knee. Despite the plethora of PRP-related citations, there is a paucity of high-level evidence that is comparable, cohort specific, dose controlled, injection protocol controlled, and double-blinded. Read More…
(RESEARCH: Treatment with platelet-rich plasma is more effective than placebo for knee osteoarthritis: a prospective, double-blind, randomized trial.)
A single dose of WBC-filtered PRP in concentrations of 10 times the normal amount is as effective as 2 injections to alleviate symptoms in early knee OA. The results, however, deteriorate after 6 months. Both groups treated with PRP had better results than did the group injected with saline only. Read More…
(ARTICLE: New York Bone and Joint – The Truth about PRP Injections, by Leon E. Popovitz, MD – Orthopaedic Surgeon.)
There has been rapidly growing interest in PRP (Platelet Rich Plasma) injections. In particular, more and more patients are interested in these novel injections for alternative, non-surgical treatment of their osteoarthritis. After all, there are so many claims from so many different health care providers about PRP. What can a patient believe? What patients can truly benefit? This review of the most relevant, true data and evidence should reveal the most vital information. Read More…